Case Overview:
One of the early survivors among 12 babies with esophageal atresia was managed by closure of the tracheoesophageal fistula (TEF), gastrostomy, and exteriorization of the cervical esophagus to the left neck as a neonate. Then a subcutaneous presternal “esophagus” was made in stages.
 n
n
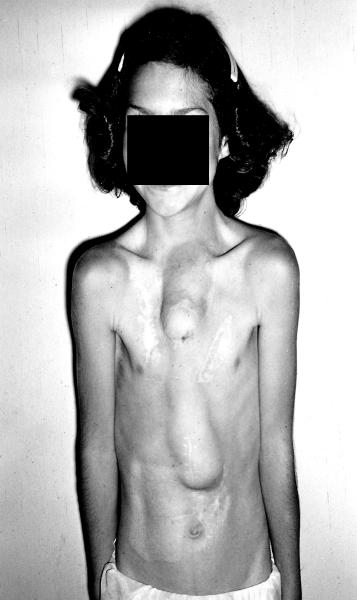
- 11-yr-old female patient born in 1944. Her first surgery was done by William Ladd, M.D., and Orvar Swenson, M.D. It included the above as an eonate plus repair of duodenal atresia. Upper presternal tube is a (skin-graft-lined) skin flap tube connected to the cervical esophagus. Lower half of the “esophagus” was a roux-en-y jejunal tube. Her swallowed food was manually massaged downward.
- In these early cases, the stomach was bypassed. They grew poorly until the stomach was functionalized.
- This child had 30 prior operations in her lifetime. I met her at age 16. A substernal colonic esophagus was constructed using left colon, antiperistaltically. The original subcutaneous tube was moved later.
- At age 19 years, large secundum atrial septal defect was closed using a dacron patch during cardiopulmonary bypass. Substernal colon was carefully removed aside to access the heart.
Follow Up:
- At age 22, she delivered a wedding invitation and casually remarked she had never experienced a menstrual period! A belated pelvic examination disclosed congenital absence of a vagina.
- Soon after the wedding, a skin graft vagina was made by Howard Ulfelder, M.D. Coitus became possible.
- At age 26, the patient and her husband adopted a baby girl.
- This patient benefitted from multiple advances made in pediatric surgery during her lifetime.
- The patient also illustrates how one malformation should prompt thorough assessment for others. She had esophageal atresia, duodenal atresia, and a cardiac defect (suspected at age 19 by hearing a loud and split-second sound via a stethoscope). On learning that she had no vagina at age 22 documents that many examiners failed to do a complete physical exam and the history takers did not include absence of menses.
THP Source:
